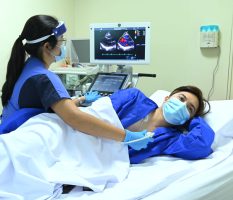
Pulmonary Institute caters to patients with:
- Restrictive lung diseases like pneumonia, neuromuscular diseases, pulmonary fibrosis and others
- Obstructive lung diseases like asthma, emphysema, bronchiectasis and others
- We also cater to patients for clearance prior to surgery and patients needing ventilatory support
SERVICES OFFERED
AEROSOL THERAPY/NEBULIZATION
It is the delivery of aerosolized medications to the airways to liquefy/hydrate dried secretions. Bronchodilators or mucolytics may be used to ease difficulty of breathing.
ULTRASONIC NEBULIZATION (USN)
Similar to nebulization however, this procedure delivers a larger volume of medication. Particles penetrate to reach the smallest airways of the lungs. This is used to hydrate and liquefy dry, retained secretions.
CHEST PHYSIOTHERAPY
The application of vibration/percussion to the chest wall to dislodge and for easier expectoration of respiratory secretions. Patient positioning may also be utilized to drain secretions by the use of gravity.
INCENTIVE SPIROMETRY (IS)
This uses visual feedback to encourage the patient to take slow, deep, sustained inspirations to improve lung function and for the prevention of alveolar collapse. This is usually requested for post thoracic and abdominal surgery patients.
INTRAPULMONARY PERCUSSIVE VENTILATION (IPPV)
A therapeutic positive pressure device used to deliver aerosolized medications and to help individuals with lung disease clear sputum. It is a combination of aerosol therapy and chest physiotherapy. It is used to assist individuals with cystic fibrosis, amyotrophic lateral sclerosis (Lou Gehrig’s disease), emphysema, and other lung ailments.
COUGH ASSIST
A non-invasive air delivery that clears secretions from the lungs by gradually applying positive and negative pressure to the airway.
OXYGEN THERAPY
This is a treatment to support the patient’s breathing by using oxygen. Helpful to hypoxemic patients. Different oxygen apparatus are used depending on the patient’s needs.
MECHANICAL VENTILATOR
A life saving device hooked to patients suffering from acute respiratory failure or other debilitating conditions to support the work of breathing .
SPONTANEOUS BREATHING PARAMETERS (SBP)
This makes use of measurement tools to determine whether the patient is ready to be weaned off the ventilator.
SPUTUM INDUCTION
This procedure is done by using the USN machine and hypertonic sodium chloride (3%) solution as medication to collect sputum for AFB staining. Hypertonic sodium chloride solution is used to irritate the airways to produce phlegm. This is usually done for 3 consecutive days.
ARTERIAL BLOOD GAS (ABG)
An invasive diagnostic test which involves blood extraction to determine the oxygenation and acid base balance of a patient. Arteries are used as site for extraction.
VENOUS BLOOD GAS
An invasive diagnostic test to determine serum bicarbonate level. This is helpful in the assessment of the kidneys. Blood is extracted from the vein. No preparation is needed.
PLEURAL FLUID pH
Using pleural fluid as sample, this test is a diagnostic predictor of the need for pleural space drainage. A pH of less than 7.2 is an indication of chest tube drainage.
PULMONARY FUNCTION TEST (PFT)
A diagnostic test to determine lung function. Patient will be asked to do different breathing maneuvers to rule out or determine the severity of restrictive or obstructive lung disease.
- Simple Spirometry
- Complete Sirometry with Lung Diffusion and Body Plethysmograph
- Impulse Oscillometry (IOS) – an alternative procedure to Simple Spirometry. This is usually requested to the very young or the very old patients who cannot execute this maneuver properly.
PULSE OXIMETRY
A non-invasive diagnostic modality which measures the patient’s oxygen saturation and pulse rate.
PEAK EXPIRATORY FLOW RATE (PEFR)
This makes use of a diagnostic device that measures the severity of airway obstruction like asthma. PEFR measurements are taken on a daily basis to detect changes in lung function. Pre and post nebulization determination may be used as basis to assess patient’s response to medication.
SLEEP STUDY (POLYSOMNOGRAPHY)
Polysomnography is a series of tests performed on patients while they sleep. It is an overnight procedure that evaluates sleep disorders. This is done on patients who have difficulty having a restful sleep at night.
BRONCHOSCOPY
Procedure in which a hollow, flexible tube called a bronchoscope is inserted into the airways through the nose or mouth to provide a view of the tracheobronchial tree. It can also be used to collect bronchial and/or lung secretions and to perform tissue biopsy.
FRACTION OF EXHALED NITRIC OXIDE (FENO) BREATH TEST
Diagnostic procedure that determines the presence of airway inflammation
CARDIO PULMONARY EXERCISE TEST (CPET)
Diagnostic procedure to evaluate the cardio pulmonary system. Both systems are consequently stressed during exercise to measure the physiologic competence of a person.
PULMONARY REHABILITATION
A supervised medical program to improve the quality of life of people with lung ailments such as Chronic Obstructive Pulmonary Disease
TUBERCULIN SKIN TEST
An invasive diagnostic procedure that will determine if the patient is infected with Mycobacterium Tuberculosis (The causative agent for Pulmonary Tuberculosis)
HIGH FLOW THERAPY
A therapeutic procedure for those patients that require a stable fraction of inhaled oxygen (FiO2) at high flow rate through a nasal cannula.
SIX MINUTE. WALK TEST
A diagnostic procedure that determines a person’s exercise tolerance. It measures how far a patient can walk in six (6) minutes